|
What is celiac disease?
Celiac disease is a
digestive disease that
damages the small intestine
and interferes with
absorption of nutrients from
food. People who have celiac
disease cannot tolerate
gluten, a protein in wheat,
rye, and barley. Gluten is
found mainly in foods but
may also be found in
everyday products such as
medicines, vitamins, and lip
balms.

The small intestine is
shaded above.
When people with celiac
disease eat foods or use
products containing gluten,
their immune system responds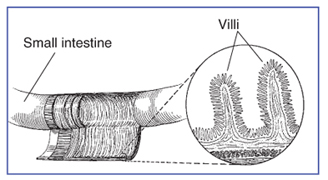 by
damaging or destroying villi�the
tiny, fingerlike protrusions
lining the small intestine.
Villi normally allow
nutrients from food to be
absorbed through the walls
of the small intestine into
the bloodstream. Without
healthy villi, a person
becomes malnourished, no
matter how much food one
eats. Villi
on the lining of the small
intestine help absorb
nutrients. by
damaging or destroying villi�the
tiny, fingerlike protrusions
lining the small intestine.
Villi normally allow
nutrients from food to be
absorbed through the walls
of the small intestine into
the bloodstream. Without
healthy villi, a person
becomes malnourished, no
matter how much food one
eats. Villi
on the lining of the small
intestine help absorb
nutrients.
Celiac disease is both a
disease of malabsorption�meaning
nutrients are not absorbed
properly�and an abnormal
immune reaction to gluten.
Celiac disease is also known
as celiac sprue, nontropical
sprue, and gluten-sensitive
enteropathy. Celiac disease
is genetic, meaning it runs
in families. Sometimes the
disease is triggered�or
becomes active for the first
time�after surgery,
pregnancy, childbirth, viral
infection, or severe
emotional stress.
What are the symptoms of
celiac disease?
Symptoms of celiac disease
vary from person to person.
Symptoms may occur in the
digestive system or in other
parts of the body. Digestive
symptoms are more common in
infants and young children
and may include
� abdominal
bloating and pain
� chronic
diarrhea
� vomiting
� constipation
� pale,
foul-smelling, or fatty
stool
� weight
loss
Irritability is another
common symptom in children.
Malabsorption of nutrients
during the years when
nutrition is critical to a
child�s normal growth and
development can result in
other problems such as
failure to thrive in
infants, delayed growth and
short stature, delayed
puberty, and dental enamel
defects of the permanent
teeth.
Adults are less likely to
have digestive symptoms and
may instead have one or more
of the following:
� unexplained
iron-deficiency anemia
� fatigue
� bone
or joint pain
� arthritis
� bone
loss or osteoporosis
� depression
or anxiety
� tingling
numbness in the hands and
feet
� seizures
� missed
menstrual periods
� infertility
or recurrent miscarriage
� canker
sores inside the mouth
� an
itchy skin rash called
dermatitis herpetiformis
People with celiac disease
may have no symptoms but can
still develop complications
of the disease over time.
Long-term complications
include malnutrition�which
can lead to anemia,
osteoporosis, and
miscarriage, among other
problems�liver diseases, and
cancers of the intestine.
Why are celiac disease
symptoms so varied?
Researchers are studying the
reasons celiac disease
affects people differently.
The length of time a person
was breastfed, the age a
person started eating
gluten-containing foods, and
the amount of
gluten-containing foods one
eats are three factors
thought to play a role in
when and how celiac disease
appears. Some studies have
shown, for example, that the
longer a person was
breastfed, the later the
symptoms of celiac disease
appear.
Symptoms also vary depending
on a person�s age and the
degree of damage to the
small intestine. Many adults
have the disease for a
decade or more before they
are diagnosed. The longer a
person goes undiagnosed and
untreated, the greater the
chance of developing
long-term complications.
What other health problems
do people with celiac
disease have?
People with celiac disease
tend to have other diseases
in which the immune system
attacks the body�s healthy
cells and tissues. The
connection between celiac
disease and these diseases
may be genetic. They include
type 1 diabetes, autoimmune
thyroid disease, autoimmune
liver disease, rheumatoid
arthritis, Addison�s
disease, a condition in
which the glands that
produce critical hormones
are damaged Sj�gren�s
syndrome, a condition in
which the glands that
produce tears and saliva are
destroyed.
How common is celiac
disease?
Celiac disease affects
people in all parts of the
world. Originally thought to
be a rare childhood
syndrome, celiac disease is
now known to be a common
genetic disorder. More than
2 million people in the
United States have the
disease, or about 1 in 133
people.1 Among people who
have a first-degree
relative�a parent, sibling,
or child�diagnosed with
celiac disease, as many as 1
in 22 people may have the
disease.2
Celiac disease is also more
common among people with
other genetic disorders
including Down syndrome and
Turner syndrome, a condition
that affects girls�
development.
How is celiac disease
diagnosed?
Recognizing celiac disease
can be difficult because
some of its symptoms are
similar to those of other
diseases. Celiac disease can
be confused with irritable
bowel syndrome,
iron-deficiency anemia
caused by menstrual blood
loss, inflammatory bowel
disease, diverticulitis,
intestinal infections, and
chronic fatigue syndrome. As
a result, celiac disease has
long been underdiagnosed or
misdiagnosed. As doctors
become more aware of the
many varied symptoms of the
disease and reliable blood
tests become more available,
diagnosis rates are
increasing.
Blood
Tests
People with celiac disease
have higher than normal
levels of certain
autoantibodies�proteins that
react against the body�s own
cells or tissues�in their
blood. To diagnose celiac
disease, doctors will test
blood for high levels of
anti-tissue transglutaminase
antibodies (tTGA) or anti-endomysium
antibodies (EMA). If test
results are negative but
celiac disease is still
suspected, additional blood
tests may be needed.
Before being tested, one
should continue to eat a
diet that includes foods
with gluten, such as breads
and pastas. If a person
stops eating foods with
gluten before being tested,
the results may be negative
for celiac disease even if
the disease is present.
Intestinal Biopsy
If blood tests and symptoms
suggest celiac disease, a
biopsy of the small
intestine is performed to
confirm the diagnosis.
During the biopsy, the
doctor removes tiny pieces
of tissue from the small
intestine to check for
damage to the villi. To
obtain the tissue sample,
the doctor eases a long,
thin tube called an
endoscope through the
patient�s mouth and stomach
into the small intestine.
The doctor then takes the
samples using instruments
passed through the
endoscope.
Dermatitis Herpetiformis
Dermatitis herpetiformis
(DH) is an intensely itchy,
blistering skin rash that
affects 15 to 25 percent of
people with celiac disease.3
The rash usually occurs on
the elbows, knees, and
buttocks. Most people with
DH have no digestive
symptoms of celiac disease.
DH is diagnosed through
blood tests and a skin
biopsy. If the antibody
tests are positive and the
skin biopsy has the typical
findings of DH, patients do
not need to have an
intestinal biopsy. Both the
skin disease and the
intestinal disease respond
to a gluten-free diet and
recur if gluten is added
back into the diet. The rash
symptoms can be controlled
with antibiotics such as
dapsone. Because dapsone
does not treat the
intestinal condition, people
with DH must maintain a
gluten-free diet.
Screening
Screening for celiac disease
means testing for the
presence of autoantibodies
in the blood in people
without symptoms. Americans
are not routinely screened
for celiac disease. However,
because celiac disease is
hereditary, family members
of a person with the disease
may wish to be tested. Four
to 12 percent of an affected
person�s first-degree
relatives will also have the
disease.
How is celiac disease
treated?
The only treatment for
celiac disease is a
gluten-free diet. Doctors
may ask a newly diagnosed
person to work with a
dietitian on a gluten-free
diet plan. A dietitian is a
health care professional who
specializes in food and
nutrition. Someone with
celiac disease can learn
from a dietitian how to read
ingredient lists and
identify foods that contain
gluten in order to make
informed decisions at the
grocery store and when
eating out.
For most people, following
this diet will stop
symptoms, heal existing
intestinal damage, and
prevent further damage.
Improvement begins within
days of starting the diet.
The small intestine usually
heals in 3 to 6 months in
children but may take
several years in adults. A
healed intestine means a
person now has villi that
can absorb nutrients from
food into the bloodstream.
To stay well, people with
celiac disease must avoid
gluten for the rest of their
lives. Eating even a small
amount of gluten can damage
the small intestine. The
damage will occur in anyone
with the disease, including
people without noticeable
symptoms. Depending on a
person�s age at diagnosis,
some problems will not
improve, such as short
stature and dental enamel
defects.
Some people with celiac
disease show no improvement
on the gluten-free diet. The
most common reason for poor
response to the diet is that
small amounts of gluten are
still being consumed. Hidden
sources of gluten include
additives such as modified
food starch, preservatives,
and stabilizers made with
wheat. And because many corn
and rice products are
produced in factories that
also manufacture wheat
products, they can be
contaminated with wheat
gluten.
Rarely, the intestinal
injury will continue despite
a strictly gluten-free diet.
People with this condition,
known as refractory celiac
disease, have severely
damaged intestines that
cannot heal. Because their
intestines are not absorbing
enough nutrients, they may
need to receive nutrients
directly into their
bloodstream through a vein,
or intravenously.
Researchers are evaluating
drug treatments for
refractory celiac disease.
|
|
What to Eat |
What NOT to Eat |
|
Flour |
Gluten & Wheat Free
Flour |
Wheat, Wholemeal,
Wholewheat & Wheatmeal
flour, Wheatbran,
Barley, Rye, Rye Flour,
Samolina, Museli. All
Baked Foods made from
Wheat , Rye, Semolina,
Barley and Pearl Barley |
|
Dairy Products |
Eggs, Milk, Cream,
Butter, Cheese, Cottage
Cheese, Curd, Coffee
Whiteners, Soya Products |
Yoghurts, Cheese Spreads |
|
Beverages |
Tea, Coffee, Herb Tea,
Aerated Drinks ( Coke,
Pepsi, Sprite etc.),
Rooh Af Zah, Fruit
Squash, Tang, Glucon D,
Cocoa, Marmite , Most
alcoholic drinks,
Pediasure |
Barley based drinks,
barley fruit drinks,
Beer, Malted drinks,
Milk Additives (Like
Nesquick, Boost, Complan
Etc.) |
|
Fruits & Vegetables |
All fruits and
vegetables unless with
certain sauces which may
contain gluten |
********* |
|
Pulses |
All except certain
brands of baked beans
and beans with a sauce
which may contain gluten |
********* |
|
Confectionary &
Sweets |
Jam, Marmalade, Sugar,
Honey, Molasses, Golden
Syrup, Some brands of
Chocolate only Wheafree,
(the ones without
any wafer filling) |
Avoid Indian sweets from
sweet shops as they may
be contaminated. Take
the ones made only in
gluten free facilities. |
|
Soups & sauces |
Many manufactured
sauces, stock cubes and
soups contain gluten |
Soya sauce needs to be
avoided unless the label
says 'Gluten Free' |
Regards
:
Sai Food
Products ( India )
|